The idea of a titanium post becoming a permanent part of your jawbone might sound like science fiction, but it’s a remarkable biological process that’s central to modern dentistry. This fusion, called osseointegration, is the secret behind the stability and longevity of dental implants. It’s also the key to understanding how do dental implants affect bone health. By physically bonding with the bone, the implant provides the stimulation needed to prevent the jaw from deteriorating after tooth loss. This guide will break down that amazing connection, explaining how an implant doesn’t just sit in your jaw—it becomes a functional part of it, protecting and preserving your bone structure for a healthy and confident smile.
Maintaining good dental health is crucial for overall well-being, and tooth loss is a common dental problem that can significantly impact a person’s quality of life. Dental implants have gained popularity as an effective solution for tooth replacement, providing a natural-looking and long-lasting alternative to traditional options like dentures and bridges. However, the success of dental implants depends on the health and quality of the jawbone. In this article, we will explore the relationship between dental implants and bone health, shedding light on the important factors that contribute to successful implantation and long-term oral health.
How Do Dental Implants Work?
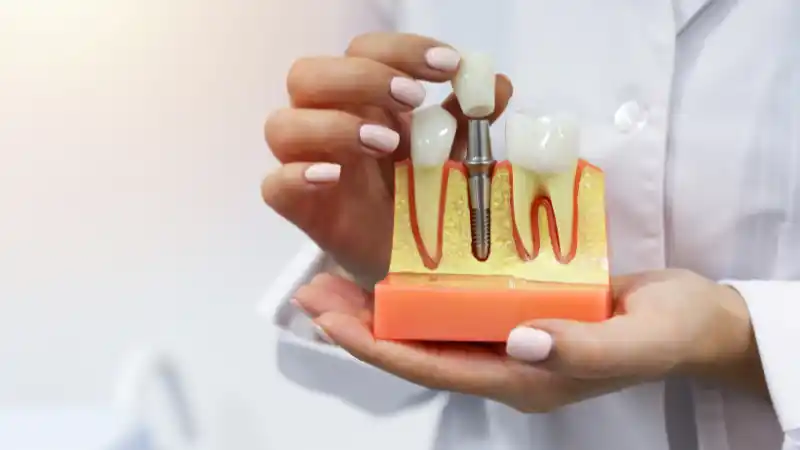
Dental implants are prosthetic tooth roots that are surgically placed into the jawbone to support artificial teeth. They consist of three main components: the implant (a titanium post), the abutment (a connector), and the dental crown (the visible tooth replacement). Dental implants mimic the function and appearance of natural teeth, providing stability, durability, and aesthetic appeal. The titanium material used in implants is biocompatible, meaning it integrates with the surrounding bone through a process called osseointegration.
Why Jawbone Health Is Key for Implants
Healthy jawbone is crucial for the success of dental implants. During osseointegration, the implant fuses with the surrounding bone, providing a stable foundation for the artificial tooth. Adequate bone density and quality are necessary to ensure proper integration and long-term stability of the implant. The jawbone needs to be able to support the forces exerted during chewing and biting. Therefore, individuals with compromised bone health may require additional procedures, such as bone grafting, to enhance bone volume and density before implant placement.
Is Your Jawbone Strong Enough for Implants?
Before undergoing dental implant treatment, a comprehensive dental examination is necessary to evaluate bone density and quality. Dentists use diagnostic tools, such as X-rays, CT scans, and cone beam computed tomography (CBCT), to assess the condition of the jawbone. These imaging techniques provide detailed information about bone volume, density, and any potential abnormalities. By thoroughly examining the bone, the dentist can determine the suitability of a patient for dental implant treatment and plan the procedure accordingly. This assessment is crucial for understanding the available bone and identifying any potential limitations or the need for additional procedures, such as bone grafting or augmentation, to ensure successful implantation.
Can You Get Dental Implants with Osteoporosis?
If you have osteoporosis and are considering dental implants, you might be wondering if it’s a safe or viable option. The short answer is yes, it is often possible to get dental implants even with osteoporosis. However, the condition does introduce some important factors that need to be carefully managed. Osteoporosis affects bone density throughout your body, including your jaw. Since dental implants rely on a strong jawbone to anchor them in place, a successful outcome requires a thoughtful approach and a skilled dental team. It’s not an automatic disqualifier, but it does mean your treatment plan will need to be tailored to your specific health needs to ensure the best possible results.
How Osteoporosis Affects the Jaw
Osteoporosis is a condition that causes bones to become less dense and more fragile. While many people associate it with the hips or spine, it can also impact the jawbone. A less dense jawbone might have a harder time supporting a dental implant and fusing with it through the process of osseointegration. This doesn’t mean the implant will fail, but it can mean the healing process is more delicate and may take longer. The primary concern is ensuring the jaw has enough strength and volume to create a stable foundation for the implant for years to come. A thorough evaluation is the first step to understanding how your bone health might influence your treatment.
Special Considerations for Implant Surgery
When you have osteoporosis, your implant surgery plan will likely include a few extra considerations. Your dental team may recommend a longer healing period after the implant is placed to give your bone more time to integrate with the titanium post. It’s also incredibly important to work with a dental implant expert who has experience treating patients with complex medical histories. An experienced specialist understands the nuances of placing implants in less-dense bone and can adapt their technique accordingly. The team at Dental & Implant Centers of Colorado is well-versed in creating customized treatment plans that account for each patient’s unique health profile, ensuring you receive specialized care.
What the Research Says
It’s helpful to know what the science says about this topic. A systematic review of studies on osteoporosis and dental implants found that while there was a slightly higher rate of implant loss in individuals with osteoporosis, the evidence wasn’t strong enough to definitively conclude that the condition prevents proper bone healing around an implant. This suggests that while caution is necessary, having osteoporosis doesn’t automatically mean your implant will fail. With careful planning and proper care from a knowledgeable team, patients with osteoporosis can and do have successful, long-lasting dental implants.
Disclosing Medications to Your Dentist
Being open with your dentist about your health history and medications is always important, but it’s especially critical if you have osteoporosis. Certain medications used to treat osteoporosis, known as bisphosphonates (like Fosamax®), can, in rare cases, lead to a serious complication called osteonecrosis of the jaw. This condition can affect healing after a surgical procedure. Providing a complete list of your medications allows your dental team to assess any potential risks and create the safest possible treatment plan for you. It’s a key step in the partnership between you and your provider, ensuring your safety and the long-term success of your implant.
Planning for Dental Implant Success
A successful dental implant journey begins long before the actual surgery. The most critical first step is a comprehensive evaluation of your oral health and, specifically, your jawbone. At Dental & Implant Centers of Colorado, we use advanced diagnostic tools like X-rays and cone beam computed tomography (CBCT) scans to get a detailed, three-dimensional picture of your jaw. This allows us to measure the bone’s density, volume, and overall quality with precision. This thorough assessment helps us determine if you are a good candidate for immediate implant placement or if you might benefit from a preparatory procedure like bone grafting to build up the area first. This meticulous planning phase is what sets the stage for a predictable, stable, and lasting outcome.
How Many Implants Will You Need?
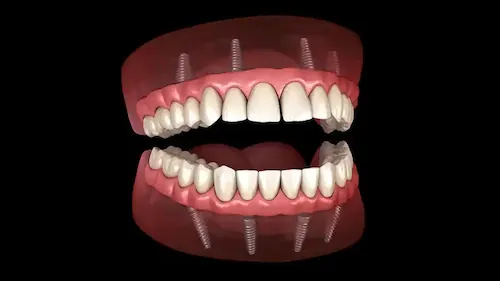
The number of implants you need depends entirely on your individual situation. If you’re missing a single tooth, one implant topped with a crown is the straightforward solution. If you have several missing teeth in a row, an implant-supported bridge might be recommended, which uses two implants to support a series of connected crowns, avoiding the need to place an implant for every single missing tooth. For those missing most or all of their teeth in an arch, a full arch restoration (sometimes called All-on-4) can replace an entire set of teeth using as few as four strategically placed implants. Your specific needs and goals will be discussed during your consultation to determine which of our dental implant services is the perfect fit for restoring your smile.
Strengthening Your Jaw with Bone Grafting
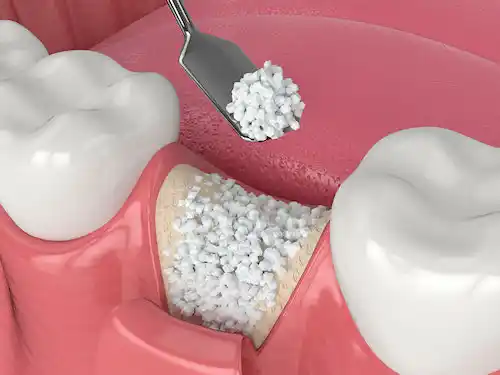
In cases where the jawbone lacks sufficient volume or density, bone grafting or augmentation procedures may be necessary before dental implant placement. Bone grafting involves transplanting bone from one area of the body, using synthetic or donated bone material, or employing growth factors to stimulate new bone growth. This procedure helps augment the jawbone and create a stable environment for successful implantation. Different types of bone grafts, such as autografts, allografts, xenografts, and alloplastic grafts, are available depending on the patient’s needs and preferences. Bone grafting can enhance bone volume, fill in defects, and improve bone density, providing a solid foundation for dental implants.
How Dental Implants Preserve Your Jawbone
Tooth loss can lead to bone resorption, a process where the jawbone gradually loses volume and density. When a tooth is missing, the surrounding bone no longer receives the stimulation it needs, causing it to deteriorate over time. This bone loss not only affects the jawbone’s structure but can also lead to changes in facial appearance, such as sunken cheeks or sagging lips. Dental implants play a crucial role in preserving bone mass. 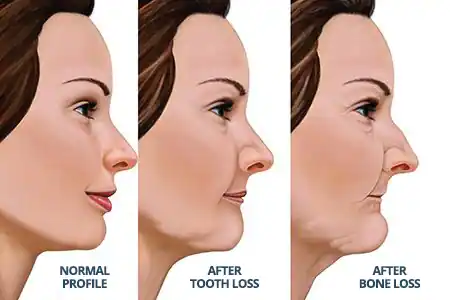
Lifestyle Factors for Preventing Bone Loss
While dental implants are a fantastic tool for preserving your jawbone, your daily habits also play a significant role in your long-term oral health. Think of it as a partnership: the implant provides the necessary stimulation, and your lifestyle choices provide the foundation for a strong, healthy jaw. Taking proactive steps to care for your bone health not only supports your implant but also contributes to your overall well-being. Simple adjustments to your diet and oral care routine can make a world of difference in ensuring your smile remains stable and secure for years to come.
Diet and Habits for Strong Bones
Building and maintaining strong bones starts from the inside out. A diet rich in calcium and vitamin D is essential for jawbone density. Think leafy greens, dairy products, and fortified foods. Just as important is what you avoid. Habits like smoking can restrict blood flow to the gums, which hinders healing and can compromise the stability of an implant. Excellent oral hygiene is also non-negotiable. Brushing twice a day, flossing daily, and attending regular check-ups are your first line of defense against infections that could threaten both your natural teeth and your implants. These consistent, healthy habits create the ideal environment for your implant to thrive.
The Importance of Timely Tooth Replacement
When you lose a tooth, the clock starts ticking on bone loss in that area. Without a tooth root to stimulate it, the jawbone begins to recede. This is why waiting too long to replace a missing tooth can complicate future treatments. Getting a dental implant promptly after losing a tooth is the most effective way to halt this process. As one study notes, implants are crucial for preserving bone mass because they “mimic natural tooth roots and transmit the forces of chewing to the jawbone.” This action signals to your body that the bone is still needed, preventing it from deteriorating and ensuring a strong foundation for your new tooth.
What if Bone Loss Occurs Around an Existing Implant?
Even with the best care, complications can sometimes arise. Discovering that you have bone loss around an existing dental implant can be concerning, but it’s important to know that it’s a treatable condition. This issue, often related to an infection called peri-implantitis, occurs when bacteria build up around the implant, leading to inflammation and the deterioration of the surrounding gum and bone tissue. The key is to catch it early. Regular dental visits and being aware of the warning signs allow your dental team to intervene quickly and effectively, protecting your investment and restoring the health of your smile.
Why Bone Loss Can Happen After Implant Placement
While dental implants have a very high success rate, certain factors can lead to bone loss after they’ve been placed. The most common culprit is an infection known as peri-implantitis, which is similar to gum disease. Poor dental hygiene is a primary cause, allowing harmful bacteria to accumulate. Other issues can also contribute; as dental experts point out, bone loss can result from an implant being placed incorrectly or experiencing too much pressure from a misaligned bite. This highlights the importance of having your implant placed by a skilled and experienced professional who can ensure proper positioning and function from the very beginning.
Warning Signs of Bone Loss Around an Implant
Your body will often give you signals if something is wrong with your dental implant. It’s crucial to pay attention to these signs so you can seek treatment right away. According to dental professionals, common warning signs of bone loss around an implant include gums that look like they are pulling back or receding from the implant crown. You might also notice that the implant feels loose, or you could experience persistent pain, swelling, or redness in the gums around it. Difficulty or discomfort while chewing is another red flag. If you notice any of these symptoms, schedule an appointment with your dentist immediately for an evaluation.
How Dentists Diagnose the Issue
If you suspect you have bone loss around an implant, your dentist will perform a thorough examination to determine the cause and extent of the problem. This process typically starts with a physical check-up to assess the health of your gums and measure the depth of the pockets around the implant. To get a clear picture of what’s happening beneath the surface, your dentist will use imaging technology. X-rays and advanced 3D scans, like a CBCT scan, are used to precisely assess the bone structure and measure how much bone has been lost, allowing for an accurate diagnosis and a carefully planned treatment approach.
Treatment Options for Peri-Implant Bone Loss
Once bone loss is diagnosed, your dentist will create a personalized treatment plan based on the severity of your condition. The primary goal is to stop the progression of the infection and, if possible, regenerate the lost bone to re-stabilize the implant. Treatment options are generally categorized as either non-surgical or surgical, with the approach depending on how far the condition has advanced.
Non-Surgical Treatments
For early-stage peri-implantitis, a non-surgical approach is often the first step. This involves a deep cleaning of the implant surface to remove the bacterial plaque and tartar that are causing the infection. Your dentist will use special tools to clean the area without damaging the implant. In some cases, this professional cleaning is combined with a course of antibiotics to eliminate the infection. Improving your at-home oral hygiene routine is also a critical component of this treatment to prevent the problem from returning.
Surgical Treatments
If the bone loss is more advanced, surgery may be necessary to save the implant. One common procedure is bone grafting, where new bone material is added to the area to rebuild the jaw and provide better support. This is often done using a technique called guided bone regeneration, which uses a special membrane to help your body grow new bone where it’s needed most. In some instances, soft tissue grafting may also be performed to restore receded gums. These surgical solutions are designed to halt the damage and create a healthy environment for your implant.
Caring for Your Implants for Lasting Results
Proper maintenance is essential to ensure the long-term success of dental implants and maintain optimal bone health. Patients should adhere to good oral hygiene practices, including regular brushing, flossing, and professional dental cleanings. It is important to attend follow-up appointments with the dentist to monitor the condition of the implant, surrounding tissues, and bone health. Dentists may recommend periodic X-rays or CBCT scans to assess the stability and integration of the implant and ensure that there are no signs of bone loss or complications. 
Initial Aftercare Tips
The first few weeks after your implant surgery are critical for a successful outcome. This is when the magic of osseointegration—the process where your jawbone fuses with the titanium implant—really begins. To give your body the best chance to heal, it’s important to follow your dentist’s instructions carefully. This usually means sticking to a soft food diet for a while to avoid putting pressure on the new implant. Think smoothies, soups, and yogurt. You’ll also want to avoid using straws, as the suction can disturb the healing site. Gentle oral hygiene is key; brush carefully around the area and use any prescribed mouth rinses to keep it clean without being too aggressive. Following these initial steps helps create a stable environment for your jawbone to heal, setting the foundation for a strong, long-lasting dental implant.
Your Next Steps Toward a Healthier Smile
Dental implants provide an effective and long-lasting solution for tooth replacement, revolutionizing restorative dentistry. Understanding the relationship between dental implants and bone health is crucial for successful implantation and maintenance of oral health. Healthy jawbone, achieved through adequate bone density and quality, is essential for the stability and longevity of dental implants. Through proper assessment, including bone density evaluations and potential bone grafting procedures, dentists can ensure optimal conditions for implant placement. By preserving bone mass and supporting the surrounding jawbone, dental implants contribute to both functional restoration and maintaining facial aesthetics. If you’re considering dental implants, consult with one of our dental professionals at Dental & Implant Centers Of Colorado for a comprehensive evaluation and personalized treatment plan to ensure the best possible outcome for your oral health. With proper care, dental implants can provide a lifetime of confident smiles and improved quality of life.
Frequently Asked Questions
How do dental implants actually help my jawbone? I thought they just replaced the tooth. While an implant beautifully fills the gap in your smile, its most important job happens below the surface. A natural tooth root stimulates your jawbone every time you chew, which keeps the bone strong and healthy. When a tooth is lost, that stimulation disappears, and the bone begins to shrink. A dental implant acts as a new root, providing that same essential stimulation and signaling to your body to maintain bone density. It becomes a functional part of your jaw, actively preserving its structure.
I’ve been missing a tooth for a long time. Is it too late for me to get an implant? It’s rarely too late, but it does mean we need to be thorough in our planning. The jawbone naturally loses some volume after a tooth has been gone for a while. The first step is always a detailed evaluation, often using 3D imaging, to see exactly how much healthy bone you have. If the area has become too thin or soft, a straightforward procedure called a bone graft can be done to rebuild a strong foundation, making the site perfect for a successful implant.
Does having low bone density or osteoporosis automatically disqualify me from getting implants? Not at all. While conditions that affect bone density require careful consideration, they don’t automatically prevent you from getting dental implants. It simply means your treatment plan will be highly customized to your specific health needs. An experienced dental team will perform a comprehensive assessment and may recommend a slightly longer healing period to ensure the implant integrates successfully with your jaw. The most important thing is to have an open conversation with your dentist about your full health history.
If I need a bone graft, what does that process actually involve? A bone graft is a common and highly predictable procedure designed to add strength and volume back to your jaw. Your dentist will place special bone grafting material into the area where the bone is deficient. This material acts like a scaffold, encouraging your body to grow new, healthy bone over several months. It’s a preparatory step that creates the solid, stable foundation necessary for a secure and long-lasting dental implant.
I already have an implant and I’m worried about it. What are the warning signs that something might be wrong? It’s always smart to pay attention to your oral health. The most common signs of a problem with an implant are similar to gum disease. Look for persistent redness, swelling, or tenderness in the gums immediately surrounding the implant. You might also notice that your gums appear to be pulling back from the implant crown or that the implant itself feels even slightly loose. If you experience any of these symptoms, schedule an appointment for an evaluation right away, as early intervention is key.
Key Takeaways
- Implants act like a workout for your jaw: By mimicking a natural tooth root, a dental implant provides the physical stimulation your jaw needs to stay strong, effectively stopping the bone loss that begins when a tooth is lost.
- Your bone health determines the starting point: A successful implant requires a solid foundation. A thorough evaluation using 3D scans will show if your jaw is ready for an implant or if a procedure like bone grafting is needed first to build it up for success.
- Daily habits are key to lasting results: While implants are durable, their long-term health depends on you. Excellent oral hygiene and regular dental check-ups are crucial for preventing infection and bone loss around the implant, protecting your smile for years to come.