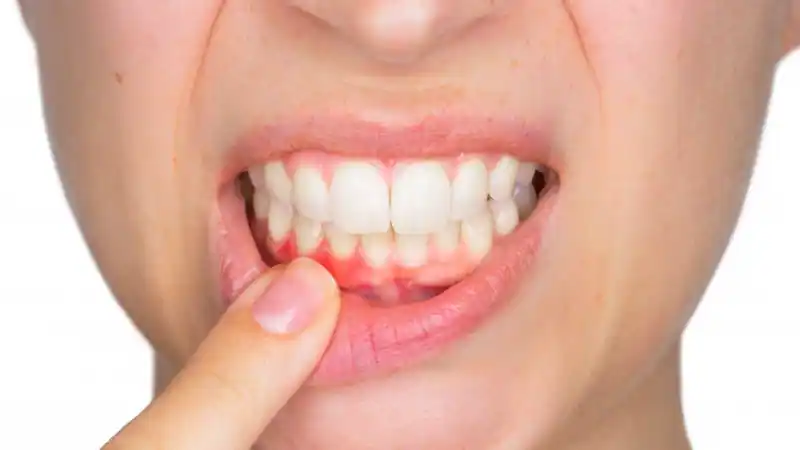
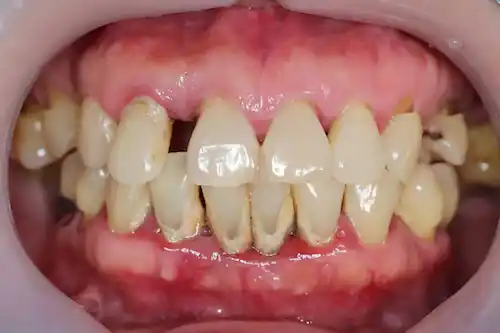
You brush twice a day, floss religiously, and never miss a dental cleaning. So why are your gums still red, swollen, or bleeding? It’s a frustrating situation, and it’s easy to feel like you’re doing something wrong. The truth is, you could have the most perfect oral hygiene routine and still be at risk. That’s because factors like genetics, hormonal changes, and other health conditions play a huge role in your gum health. If you have a family history of tooth loss, you may be predisposed to Periodontal Disease, a serious gum infection that can damage tissue and bone. Understanding that it’s not always about how well you brush is the first step toward getting the right kind of help.
Are you someone who follows a diligent oral hygiene routine, but has still had to seek treatment for gum disease? Even those who consistently brush and floss, eat a healthy diet, and attend all dental appointments may find themselves struggling with periodontal disease, and it may not be due to their own actions. In fact, genetics may be a contributing factor. Research suggests that up to 30% of the population may have a genetic predisposition to gum disease, which, if left untreated, can result in tooth and bone loss. This means that if your parents or grandparents have experienced tooth loss or gum disease, it is important for you to maintain regular visits to the dentist in order to ensure the health of your mouth. Dental & Implant Centers Of Colorado in Denver has a team of skilled periodontists who specialize in treating various types of gum disease. Given that gum disease can be influenced by numerous factors, it is crucial for individuals with a family history of the condition to seek the expertise of a periodontist to ensure their oral health is maintained. To initiate periodontal treatment, a diagnosis must first be made. This entails a clinical examination, including X-rays, and a comprehensive review of your medical and dental history by your dentist or periodontist. If you have knowledge of a family history of gum disease, it is important to inform your periodontist. In the event that you have a history of gum disease or a family history of it, your periodontist can closely monitor your oral health and develop a customized plan to prevent any further deterioration of your teeth and gums. Periodontal disease is a result of the interplay between bacteria and the body’s immune system. While some individuals may be fortunate enough to fend off bacterial infections, even with suboptimal oral hygiene, others may struggle to do so, regardless of how meticulously they brush and floss. Individuals who may have a genetic predisposition for gum disease should be particularly diligent in maintaining a proper oral care routine and seeing a gum disease specialist regularly. Providing a complete medical history, including any family history of the condition, will enable your periodontist to develop an accurate treatment plan tailored to your unique needs and susceptibility to the disease. If you experience any of the following symptoms, it is important to schedule an appointment with a periodontist promptly:
- Bleeding gums while brushing and flossing
- Red, swollen, or tender gums
- Bad breath
- Receding gums or gums that are pulling away from the teeth
- Teeth that are loose or shifting
- Changes in your bite or in the fit of your partial dentures.
What is Periodontal Disease?
Periodontal disease, more commonly known as gum disease, is a serious infection that damages the soft tissue and bone supporting your teeth. It’s caused by bacteria in plaque, that sticky film that constantly forms on your teeth. If left untreated, this condition can progress from simple gum inflammation to major damage, eventually leading to tooth loss. Think of it as a quiet but persistent problem that starts small but can have significant consequences for your oral and overall health. Understanding what it is and how it develops is the first step toward preventing it or managing it effectively. The good news is that with the right care and professional guidance, you can protect your smile for years to come.
Understanding the Disease and Its Progression
At its core, periodontal disease is an inflammatory response to a bacterial infection below the gumline. When plaque isn’t removed through daily brushing and flossing, it builds up and hardens. The bacteria in this plaque release toxins that irritate the gums, causing your immune system to kick into gear. This immune response, combined with the bacterial toxins, starts to break down the bone and connective tissue that hold your teeth in place. The disease progresses over time, often without much pain in the early stages, which is why regular dental check-ups are so important. Catching it early can make all the difference in the outcome of your treatment and the long-term health of your mouth.
The Stages of Gum Disease: Gingivitis and Periodontitis
Gum disease isn’t a single condition; it progresses through distinct stages. The earliest stage is gingivitis, which is simply an inflammation of the gums. You might notice that your gums are red, swollen, or bleed easily when you brush. The key thing to know about gingivitis is that it’s completely reversible with good oral hygiene and professional cleanings. However, if left untreated, it can advance to periodontitis. This is a much more serious stage where the gums pull away from the teeth, forming infected pockets. As the disease worsens, the bone and tissues supporting the teeth are destroyed, which can cause teeth to become loose and eventually fall out or require extraction.
Is Gum Disease Curable?
This is a common and important question. The answer depends on the stage of the disease. Gingivitis, the initial stage, is curable. By stepping up your brushing and flossing game and getting a professional cleaning, you can reverse the inflammation and restore your gums to full health. Once the disease progresses to periodontitis and bone loss has occurred, it is no longer considered curable. However, it is absolutely manageable. With proper professional treatment and a diligent at-home care routine, you can halt the progression of the disease and maintain a healthy mouth for the rest of your life. The goal shifts from curing the disease to controlling it and preventing further damage.
Causes and Key Risk Factors
While the direct cause of gum disease is bacterial plaque, several other factors can significantly increase your risk of developing it. It’s not always as simple as just needing to brush more. Understanding these risk factors is crucial because it helps you and your dental team create a more effective prevention and treatment strategy. Some of these factors are within your control, like your oral hygiene habits and lifestyle choices, while others, such as your genetic makeup, are not. Recognizing your personal risk profile allows you to be more proactive in protecting your gums and teeth from this progressive disease.
The Primary Cause: Plaque and Tartar
The main culprit behind gum disease is plaque. Plaque is a sticky, colorless film packed with bacteria that constantly forms on your teeth. If you don’t remove it daily through brushing and flossing, it continues to accumulate. Within just a day or two, this plaque can harden into tartar, also known as calculus. Unlike plaque, tartar is a hard, mineralized deposit that can’t be brushed away at home. It can only be removed by a dental professional during a cleaning. Tartar buildup along and under the gumline acts as a rough surface that attracts even more plaque, creating a vicious cycle of irritation and inflammation that leads to gum disease.
Major Risk Factors
Beyond the primary cause of plaque, certain factors can make you more susceptible to developing periodontal disease or make an existing condition worse. These risk factors can weaken your body’s defenses, accelerate bone loss, or create an environment where harmful bacteria thrive more easily. Some people can have excellent oral hygiene and still face challenges due to these underlying issues. Identifying and addressing these risk factors is a key part of a comprehensive approach to managing your oral health and preventing the long-term damage associated with advanced gum disease.
Genetics
You can do everything right—brush twice a day, floss daily, and never miss a dental appointment—and still find yourself at a higher risk for gum disease. Why? It might be in your genes. Research suggests that a significant portion of the population may have a genetic predisposition to periodontal disease. This means that your unique genetic makeup can affect how your immune system responds to the bacteria in plaque. If your parents or other close relatives have a history of gum disease or tooth loss, it’s a good idea to be extra vigilant with your own oral health and let your dentist know about your family history.
Smoking and Tobacco Use
If there’s one lifestyle choice that is overwhelmingly linked to gum disease, it’s smoking. In fact, smoking is considered the most significant risk factor for the development and progression of periodontitis. Not only does it weaken your immune system, making it harder to fight off gum infections, but it also reduces blood flow to the gums, which slows down healing. This means that if you’re a smoker, you’re more likely to get gum disease, and treatments are often less successful. Quitting smoking is one of the best things you can do for your gums and your overall health.
Other Contributing Factors
Several other health conditions and life stages can influence your gum health. Diabetes is a major factor, as it can reduce the body’s ability to fight infection, including infections in your gums. Hormonal changes, such as those during pregnancy or menopause, can make gums more sensitive and prone to inflammation. Chronic stress can also impair your immune response. Additionally, certain medications, like some antidepressants and heart medicines, can cause dry mouth, which allows plaque to build up more easily. This is why a holistic approach that considers your entire health profile is so important for effective dental care.
Measuring Gum Pockets
During a dental exam, one of the first steps in checking for gum disease is measuring the space between your teeth and gums. This space is called a periodontal pocket. Your dentist or hygienist will use a tiny ruler, called a probe, to gently measure the depth of these pockets. In a healthy mouth, these pockets are typically between 1 and 3 millimeters deep. If the probe indicates deeper pockets, it’s often a sign that gum disease has started to progress, creating more space for harmful bacteria to accumulate. This simple, painless measurement gives your dental team a clear picture of your gum health and helps determine the best course of action to keep your smile healthy and strong.
Professional Treatment Options
If your dentist diagnoses you with gum disease, don’t worry—there are highly effective ways to manage it. The primary goal of any treatment is to halt the infection in its tracks and prevent it from causing more damage to your gums and the bone supporting your teeth. The right approach for you will depend entirely on how advanced the disease is. For early stages, less invasive methods are often enough. For more advanced cases, a more comprehensive plan may be needed. At Dental & Implant Centers of Colorado, our team creates a personalized treatment plan tailored to your specific situation. Success is a team effort; the professional services we provide combined with your commitment to daily oral hygiene at home are the keys to getting your gum health back on track and maintaining it for the long haul.
Non-Surgical Treatments
For the earlier stages of gum disease, non-surgical treatments are the first line of defense. If you have gingivitis, the mildest form, a professional dental cleaning and a renewed focus on your daily brushing and flossing routine can often reverse the condition. For gum disease that has progressed slightly, a deep cleaning procedure called scaling and root planing is recommended. During this treatment, your hygienist or dentist will carefully remove plaque and tartar from above and below the gumline (scaling) and then smooth out the tooth roots (planing). This helps the gums reattach to the teeth and eliminates the rough spots where bacteria love to hide.
Surgical Treatments
When gum disease is more advanced, surgical options may be necessary to restore your oral health. One common procedure is pocket reduction surgery, also known as flap surgery. In this treatment, the gums are gently lifted back so your periodontist can remove deep-seated tartar and smooth damaged bone. The gums are then stitched back into place, fitting more snugly around the tooth. If significant bone has been lost, a bone graft may be performed. This involves placing special material in the area of bone loss to encourage your body to regenerate its own bone, providing a stronger foundation for your teeth or for future dental implants.
Prevention and Home Care for Healthy Gums
While professional treatment is key to managing periodontal disease, what you do at home every day forms the foundation of your oral health. Think of your daily routine as the first line of defense against harmful bacteria. The primary goal of any gum disease treatment is to control the infection, and its success heavily relies on your commitment to excellent at-home care. Partnering with your dental team and maintaining these habits can make a significant difference in stopping the progression of the disease and keeping your gums healthy for the long term. It’s about creating a consistent routine that disrupts plaque before it has a chance to cause serious damage.
Essential At-Home Care Steps
Your daily habits are powerful tools in the fight against gum disease. Brushing your teeth for two minutes, twice a day, is non-negotiable for removing plaque and food debris from the surfaces of your teeth. Just as important is flossing at least once a day to clean the tight spaces between your teeth and under the gumline, where your toothbrush can’t reach. You might also consider adding an antimicrobial mouthwash to your routine to help reduce bacteria. These simple steps, when performed consistently, disrupt the bacterial colonies that lead to inflammation and infection, playing a crucial role in preventing the onset or progression of periodontal disease.
The Importance of Quitting Tobacco
If you use tobacco, quitting is one of the most impactful things you can do for your gum health. Smoking is a major risk factor for developing periodontal disease because it weakens your body’s immune system, making it harder to fight off gum infections. It also slows down healing, which can make treatments less effective. Smokers are more likely to have calculus form on their teeth, develop deeper periodontal pockets, and lose more bone as the disease advances. Making the decision to quit smoking can dramatically improve your body’s ability to heal and respond to periodontal therapy, giving you a much better chance at successfully managing the condition.
Regular Professional Cleanings
Even the most diligent at-home care routine can’t remove everything. Plaque that isn’t removed can harden into tartar (or calculus), a stubborn substance that can only be eliminated with professional instruments. That’s why regular dental cleanings are so important. For most people, a cleaning every six to 12 months is sufficient. However, if you have risk factors like smoking, dry mouth, or a history of gum disease, you may need more frequent visits. At the Dental & Implant Centers of Colorado, our team can assess your specific situation and recommend a cleaning schedule designed to keep your gums healthy and prevent future problems.
Important Facts About Periodontal Disease
Understanding the facts about periodontal disease can help you grasp its significance and motivate you to prioritize your oral health. It’s not just a minor issue of bleeding gums; it’s a chronic inflammatory condition with potential effects on your overall well-being. Knowing how common it is and how it can be transmitted can shift your perspective from seeing it as a personal failing to recognizing it as a widespread health issue that requires professional attention. This knowledge empowers you to take proactive steps for yourself and to have more informed conversations with your family and your dental care providers about prevention and treatment.
How Common is Gum Disease?
If you’ve been diagnosed with gum disease, you are far from alone. Statistics show that nearly half of all adults over the age of 30 in the United States have some form of periodontal disease. This number increases with age, affecting over 70% of adults 65 and older. The prevalence of this condition highlights that it’s a common health problem, not something to be embarrassed about. Instead, it underscores the importance of regular dental check-ups for early detection and treatment. Recognizing how widespread it is can encourage more people to seek the care they need without feeling isolated in their diagnosis.
Can Gum Disease Bacteria Spread?
Many people are surprised to learn that the bacteria responsible for causing gum disease can be passed from one person to another. This transmission typically occurs through saliva, meaning activities like kissing or sharing utensils and toothbrushes over a prolonged period can spread these specific oral bacteria. While this doesn’t mean you’ll automatically get gum disease if a loved one has it, it does mean you could be at a higher risk, especially if you have other contributing factors. This makes it even more important for everyone in a household to practice good oral hygiene and see a dentist regularly. If you have concerns, our experienced team can provide guidance for your entire family.
Can You Get Dental Implants If You Have Periodontal Disease?
Periodontal disease can impact the success of dental implants, which are artificial tooth roots placed into the jawbone to support replacement teeth or bridges. If gum disease is left untreated, it can result in the destruction of the jawbone and ultimately cause the implants to loosen and fail. Additionally, individuals with a history of gum disease may require additional treatment and monitoring to ensure the longevity of their implants. Therefore, maintaining good oral hygiene, receiving regular dental checkups, and promptly addressing any signs of periodontal disease are essential for preserving the health of both natural teeth and dental implants. Dental implants are not a treatment for periodontal disease. While dental implants can replace teeth lost due to periodontal disease, they do not address the underlying infection and inflammation that cause the disease. In fact, individuals with periodontal disease may not be good candidates for dental implants until the disease is brought under control. It is important to seek treatment for periodontal disease as soon as possible to prevent further damage to the teeth and gums and to determine the appropriate course of action for restoring your dental health.
Frequently Asked Questions
I brush and floss every day. Why do I still have gum problems? It’s incredibly frustrating to do everything right and still have issues, but it’s often not about your routine. Genetics play a significant role in your susceptibility to gum disease. Your unique immune response to bacteria is inherited, meaning if your family has a history of tooth loss or gum problems, you might be at a higher risk regardless of how well you care for your teeth. This is why professional guidance is so important—we can create a plan that accounts for your personal risk factors.
My gums only bleed a little when I brush. Should I really be concerned? Yes, you should see it as an important warning sign. Bleeding gums are never normal; they are the earliest indicator of gum inflammation, known as gingivitis. While gingivitis is completely reversible with professional cleaning and diligent home care, ignoring it allows it to progress into more serious, irreversible periodontitis. Think of it as your body’s way of telling you to pay attention before a small problem becomes a major one.
Once I get treatment, is my gum disease cured for good? This depends on the stage of your condition. If you catch it at the earliest stage, gingivitis, it can be completely cured and reversed. However, once the disease progresses to periodontitis and causes bone loss, it is no longer considered curable. The good news is that it is absolutely manageable. Through professional treatment and consistent at-home care, we can halt the disease’s progression and prevent further damage, allowing you to maintain a healthy mouth for life.
I’ve already lost a tooth from gum disease. Can I get a dental implant? It’s possible, but the first priority is to get the gum disease under control. Placing a dental implant in an unhealthy mouth is like building a house on an unstable foundation—it’s destined to fail. Before considering an implant, we must treat the active infection and ensure your gums and jawbone are healthy enough to support it. Once your periodontal health is stable, a dental implant can be an excellent solution for replacing a lost tooth.
Is it true that I can get gum disease from my partner? The specific bacteria that cause periodontal disease can be transmitted through saliva. This means that activities like kissing or sharing a toothbrush can transfer these bacteria from one person to another. While this doesn’t guarantee you’ll develop the disease, it can increase your risk, especially if you have other contributing factors like a genetic predisposition. It highlights why it’s important for everyone in a household to maintain good oral hygiene and see a dentist regularly.
Key Takeaways
- Your Risk Isn’t Just About Hygiene: Even with perfect brushing and flossing, factors like your family history, smoking, or other health conditions can make you more susceptible to gum disease. Be sure to share your complete health profile with your dentist.
- Act Quickly to Control the Damage: The earliest stage of gum disease, gingivitis, is reversible. While more advanced periodontitis isn’t curable, it is absolutely manageable with professional treatment designed to stop its progression and protect your teeth.
- Consistent Care is a Team Effort: Professional treatments are essential for getting gum disease under control, but long-term success hinges on your daily at-home routine and sticking to a schedule of regular professional cleanings.