One of the biggest myths in dentistry is that you can’t get dental implants if you’ve had serious gum disease. This belief prevents many people from exploring a life-changing solution for missing teeth. Let’s set the record straight: you absolutely can get implants, but we have to address the gum disease first. The success of dental implants and periodontal disease management hinges on creating a healthy oral environment before the procedure begins. This article breaks down the facts, explaining the necessary steps like treating active infections, assessing bone health, and the critical role of ongoing maintenance to ensure your new smile is built to last.
Periodontal Disease and Dental Implants
What Is Periodontal Disease?
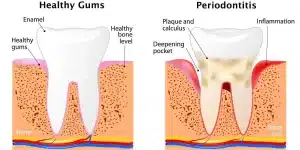
Periodontal disease, commonly referred to as gum disease, is a progressive infection of the gums and supporting structures of the teeth. It is one of the leading causes of tooth loss in adults. The condition begins with bacterial plaque accumulation around the teeth and, if untreated, advances to destroy the gum tissue and underlying bone. Over time, periodontal disease can severely impact your oral health and quality of life. What makes periodontal disease particularly concerning is that it often goes unnoticed in its early stages. Many individuals experience mild symptoms such as gum inflammation or bleeding and dismiss them as insignificant. This lack of awareness allows the disease to progress silently, causing irreversible damage. For those who lose teeth due to this condition, dental implants can offer a durable and effective solution.
What Gum Disease Really Does to Your Mouth
The damage caused by periodontal disease is not limited to the gums. As the infection advances, it spreads to the bone that supports the teeth, leading to its gradual deterioration. Without sufficient bone support, teeth become loose and may eventually fall out. Furthermore, the bacteria involved in periodontal disease can enter the bloodstream, contributing to systemic health problems such as cardiovascular disease, diabetes, and respiratory infections. Beyond its physical effects, periodontal disease also takes an emotional toll. Tooth loss can lead to a lack of confidence, difficulties with speech, and challenges in eating. Fortunately, dental implants can address these issues by restoring both the function and aesthetics of your smile.
Simple Ways to Prevent Gum Disease
Preventing periodontal disease is entirely possible with a commitment to good oral hygiene and regular dental visits. Prevention not only protects your teeth and gums but also ensures a strong foundation for treatments like dental implants, should they become necessary in the future.
Daily Habits for Healthy Gums
- Brushing: Brush your teeth at least twice a day using fluoride toothpaste. Make sure to clean along the gumline, as this is where plaque often accumulates.
- Flossing: Daily flossing is essential to remove debris and plaque from between your teeth and below the gumline, areas your toothbrush cannot reach.
- Mouthwash: Antibacterial mouthwashes can reduce harmful bacteria and freshen your breath, providing an extra layer of protection against gum disease.
- Dietary Choices: A balanced diet rich in vitamins C and D, calcium, and antioxidants strengthens your immune system and supports gum health.
- Avoid Smoking: Smoking weakens your immune system and impairs your body’s ability to fight off infections, significantly increasing the risk of gum disease.
- Dental Checkups: Professional cleanings and dental exams are crucial for identifying and addressing early signs of periodontal disease.
Recognizing the Warning Signs of Gum Disease
Identifying the symptoms of periodontal disease early is critical for effective treatment. The condition progresses through stages, with symptoms becoming more severe as the disease advances.
Early Warning Signs to Watch For
- Red, swollen, or tender gums
- Gums that bleed easily during brushing or flossing
- Persistent bad breath or a metallic taste in the mouth
Signs the Disease Is Progressing
- Receding gums that expose more of the tooth
- Loose or shifting teeth
- Painful chewing or sensitivity
- Pus-filled pockets around the gums
Your Treatment Options for Gum Disease
The treatment of periodontal disease depends on the severity of the condition. In its early stages, non-surgical interventions can be highly effective, while advanced cases may require surgical procedures and tooth replacement options such as dental implants.
Starting with Non-Surgical Options
Non-surgical treatments focus on eliminating the infection and preventing further progression of the disease. These include:
- Scaling and Root Planing: This deep cleaning procedure removes plaque and tartar from below the gumline and smooths the tooth roots to discourage bacterial growth.
- Antibiotics: Topical or oral antibiotics may be used to target and reduce bacterial infection.
Surgical Solutions for Advanced Gum Disease
Advanced periodontal disease often requires surgical intervention to repair damage and restore oral health. Surgical options include:
- Gum Grafts: Replacing lost gum tissue to protect exposed tooth roots.
- Bone Grafts: Restoring lost bone to provide a stable foundation for dental implants.
- Pocket Reduction Surgery: Reducing the depth of gum pockets to limit bacterial accumulation.
The Role of a Periodontist
When you’re considering dental implants, especially if you have a history of gum disease, a periodontist is an essential part of your care team. Think of them as a specialist for your gums and the foundation of your teeth. They have advanced training in preventing, diagnosing, and treating periodontal disease, as well as in the precise placement of dental implants. Before you can even begin the implant process, any active gum disease must be fully treated. A periodontist ensures your gums and jawbone are healthy and strong enough to provide a stable base for your new implant, setting you up for the best possible outcome.
Their expertise is crucial not just for placing the implant, but for its long-term success. A periodontist manages complex cases and helps maintain the health of the tissues surrounding the implant for years to come. Should any issues arise after your procedure, like an infection, they are the specialists equipped to handle it. Having direct access to this level of specialized care is a major advantage. At Dental & Implant Centers of Colorado, our multi-specialty approach means you can work with experts like our on-staff periodontist, ensuring comprehensive care every step of the way. You can meet the team of specialists dedicated to restoring your smile.
Can You Get Dental Implants After Gum Disease?
Dental implants are a transformative solution for individuals who have lost teeth due to periodontal disease. Unlike dentures or bridges, implants are anchored directly into the jawbone, mimicking the function of natural tooth roots. This not only provides unparalleled stability but also helps maintain bone density by stimulating natural bone growth. For patients with a history of periodontal disease, ensuring that the gums and jawbone are healthy before implant placement is critical. In cases of significant bone loss, bone grafting may be required to prepare the jaw for implant surgery. Once the implants are placed, they can restore both the function and appearance of the smile, allowing patients to eat, speak, and live with confidence.
The First Rule: Treating Active Gum Disease
Before we can even talk about implants, we have to address the root of the problem: the gum disease itself. Think of it like building a house—you wouldn’t start construction on a shaky, unstable foundation. The same principle applies to your mouth. Placing a dental implant in an area with active periodontal disease is a setup for failure, as the infection can compromise the implant’s ability to integrate with your jawbone. The first and most critical step is to get the gum disease under control. This means working with a dental professional to eliminate the infection and restore your gums to a healthy state. Only after your gums are healthy can we begin planning for a successful and long-lasting dental implant.
Assessing Your Candidacy: The 3/2 Rule
Once your gums are healthy, the next step is to evaluate the condition of your jawbone. Gum disease often causes significant bone loss, which can affect your eligibility for implants. To ensure a successful outcome, dentists follow a crucial guideline known as the “3/2 rule.” This rule specifies that there must be at least 3 millimeters of bone on the front (cheek-facing) side of the implant and at least 2 millimeters of healthy gum tissue between the implant and the adjacent teeth. This precise measurement ensures the implant has enough support to remain stable for years to come and helps create a natural-looking result. Following this standard is a key part of how our expert team ensures predictable, high-quality outcomes for our patients.
How Bone Grafting Prepares You for Implants
What happens if you don’t have enough bone to meet the 3/2 rule? Don’t worry, this doesn’t automatically disqualify you from getting implants. For many patients, a procedure called bone grafting is the solution. A bone graft involves adding new bone material to your jaw where it has deteriorated. This new material acts as a scaffold, encouraging your body to grow new, strong bone in that area. After the procedure, your jaw will need time to heal, typically around four to six months, allowing the new bone to become fully integrated and strong. Bone grafting is a common and highly successful procedure that has made it possible for countless people to rebuild their foundation and become excellent candidates for dental implants.
Protecting Your Investment: Implant Care and Risks
Choosing to get dental implants is a major step toward restoring your smile and improving your quality of life. It’s an investment in your health, confidence, and overall well-being. Like any valuable investment, your implants require consistent care to ensure they last a lifetime. While implants are designed to be a permanent solution, they aren’t invincible. The health of the surrounding gum and bone tissue is crucial for their long-term success. Understanding how to care for them properly and recognizing potential risks is the best way to protect your new smile and enjoy its benefits for years to come.
Understanding Peri-Implantitis: Gum Disease for Implants
You might be surprised to learn that dental implants can get infections, even though the implant itself is made of artificial material. This condition is called peri-implantitis, and it’s essentially the implant equivalent of gum disease. It occurs when bacteria build up around the base of the implant, leading to inflammation in the surrounding gum tissue. If left untreated, this infection can progress and start to destroy the jawbone that holds the implant securely in place. This bone loss can cause the implant to become loose and, in severe cases, fail completely. Recognizing this risk is the first step toward prevention.
Why Implants Are Vulnerable
Natural teeth have a built-in defense mechanism that implants lack. They are attached to the jawbone by a periodontal ligament, a tiny layer of tissue that acts as a shock absorber and provides a protective barrier against bacterial infection. Dental implants, on the other hand, fuse directly to the bone in a process called osseointegration. While this creates a very strong bond, it also means there’s no ligament to help shield the bone from bacteria. This makes the area around an implant more susceptible to rapid bone loss if an infection like peri-implantitis takes hold.
Causes and Warning Signs of Implant Infections
Peri-implantitis is most often caused by inadequate oral hygiene, which allows harmful plaque to accumulate around the implant. However, other factors can increase your risk, including a history of severe gum disease, smoking or vaping, and uncontrolled health conditions like diabetes. It’s important to be aware of the warning signs so you can seek help early. Keep an eye out for gums that bleed when you brush or floss, look red or swollen around the implant, or feel tender. Other signs include gums pulling back and exposing the implant, persistent bad breath, or a bad taste in your mouth.
Long-Term Maintenance for Lasting Success
The good news is that with the right care, you can significantly reduce your risk of complications and ensure your implants thrive for decades. Think of long-term maintenance as a partnership between you and your dental team. Your daily habits at home are the foundation of implant health, while regular professional check-ups provide the expert oversight needed to catch any potential issues before they become serious. This combination of personal diligence and professional care is the key to making your dental implant journey a lasting success.
The Importance of Professional Cleanings
Even if you’re a brushing and flossing superstar, you can’t remove everything on your own. Plaque can harden into tartar, which can only be removed with special instruments during a professional cleaning. We recommend visiting your dentist for cleanings and exams at least twice a year. During these appointments, our team will not only clean around your implant but also check its stability, assess the health of your gums, and take X-rays to monitor your bone levels. These regular visits allow us to ensure everything is functioning perfectly and to provide the specialized care your investment deserves.
At-Home Care: Tools and Techniques
Your daily cleaning routine is your first line of defense against implant problems. You’ll need to brush twice a day and clean between your teeth daily, just as you would with natural teeth. However, you may need some special tools to effectively clean around the implant crown. Many patients find that interdental brushes, which are small brushes designed to fit between teeth, or water flossers are excellent for removing plaque and food debris from the tricky areas around an implant. Your hygienist can show you the best techniques and tools for your specific situation.
Modern Treatments for Implant Complications
If you do notice any warning signs of an infection, don’t panic. Peri-implantitis is treatable, and the outcome is often excellent, especially when it’s addressed early. The goal of treatment is to stop the progression of the infection and preserve the bone supporting the implant. Depending on the severity, treatment might involve a deep cleaning of the implant surface, the use of antibiotics, or advanced techniques like laser therapy to disinfect the area. At Dental & Implant Centers of Colorado, we offer a comprehensive range of dental services to manage any complications and keep your smile healthy.
More Than Just a Smile: Gum Health and Your Body
Periodontal disease is not just an oral health issue—it has been linked to systemic health conditions such as diabetes, heart disease, and respiratory infections. Chronic inflammation caused by gum disease can have far-reaching effects on the body, emphasizing the importance of timely treatment. By addressing gum disease and restoring missing teeth with dental implants, patients can improve their overall health and reduce the risk of developing related conditions. This holistic approach to care highlights the interconnectedness of oral and systemic health.
The Advantages of Implants for Gum Disease Patients
For individuals recovering from periodontal disease, dental implants offer numerous benefits, including:
- Longevity: With proper care, dental implants can last a lifetime, making them a cost-effective solution over time.
- Functionality: Implants allow patients to chew and speak naturally, restoring their quality of life.
- Aesthetics: Custom-designed crowns blend seamlessly with natural teeth, creating a beautiful smile.
- Bone Preservation: Implants stimulate bone growth, preventing further bone loss and maintaining facial structure.
Success Rates: What the Data Shows
If you’re wondering whether dental implants are a safe bet after battling gum disease, you can breathe a sigh of relief. The answer is a definite yes, with a small but important catch. Studies show that dental implants have a high success rate in patients with a history of periodontitis, as long as the active gum disease is completely resolved before the procedure. This isn’t a one-and-done fix; think of it as a partnership. Because of your history, you’ll have a higher risk of issues like inflammation, so diligent home care and consistent professional cleanings are non-negotiable. Protecting your investment means keeping the surrounding gums healthy—that’s the key to making your new smile last a lifetime.
Your Next Steps Toward a Healthier Smile
Periodontal disease is a serious condition that can lead to tooth loss and systemic health issues if left untreated. However, with early detection, effective treatment, and the use of dental implants, patients can regain their oral health and confidence. Dental implants not only restore the function and appearance of your smile but also provide long-term benefits for your overall well-being. If you are struggling with the effects of periodontal disease, consult with a dental professional to explore your options. Dental implants may be the key to a healthier, happier future.
Frequently Asked Questions
If I’ve lost teeth to gum disease, am I automatically disqualified from getting dental implants? Not at all. This is one of the biggest misconceptions we hear. Having a history of periodontal disease doesn’t rule you out for implants. The most important factor is that any active infection must be completely treated and your gums must be healthy before we begin the implant process. Think of it as creating a stable, healthy foundation before building your new smile.
What if gum disease has damaged my jawbone? Can I still get an implant? Yes, this is a very common situation, and there are excellent solutions. Periodontal disease often leads to bone loss, but that doesn’t mean an implant is impossible. A procedure called bone grafting can be used to rebuild the lost bone in your jaw, creating the strong support structure needed for a successful implant. This is a routine and highly effective way to prepare you for the procedure.
Are dental implants more likely to fail if I have a history of periodontal disease? Your risk is slightly higher, but failure is absolutely not a given. The success of your implant comes down to a partnership between you and your dental team. Because you’ve been susceptible to gum disease before, you’ll need to be extra diligent with your home care and stick to a regular schedule of professional cleanings. With consistent maintenance, your implant can last a lifetime.
How is caring for a dental implant different from a natural tooth, especially after having gum disease? While the implant itself can’t get a cavity, the gum and bone tissue around it can still get infected—a condition called peri-implantitis. Because implants don’t have the natural protective barrier that teeth do, it’s crucial to keep the area clean. Your daily routine will be similar—brushing twice a day and cleaning between your teeth—but you might use special tools like a water flosser or interdental brushes to effectively clean around the implant.
What’s the first step in the process if I want to explore implants but I’m worried about my gum health? The first step is to schedule a consultation. During this visit, we’ll assess the current health of your gums and jawbone. If there’s any active gum disease, we’ll create a personalized treatment plan to resolve it. Once your mouth is healthy, we can then determine the best path forward for placing your dental implants and restoring your smile.
Key Takeaways
- A Healthy Foundation is the First Priority: You can get dental implants even with a history of gum disease, but the active infection must be fully treated first. Creating a healthy, stable environment for the implant is the most critical step for long-term success.
- Bone Support is Key (And It Can Be Restored): Implants need a certain amount of jawbone to anchor them securely. If gum disease has caused bone loss, a common and effective procedure like bone grafting can rebuild that foundation, making you an excellent candidate.
- Implants Require Lifelong Care: To prevent an implant-specific infection called peri-implantitis, your new tooth requires diligent care. A commitment to excellent at-home hygiene and regular professional cleanings is essential to protect your investment for a lifetime.